GamMed Mission – The Gambia, March 2026
Introduction
In March 2026, following an invitation from the BFIRST Chairman, Mr Tony Barabas, I joined the GamMed (Gambia Medical UK Partnership) surgical mission to Banjul, The Gambia. The team departed from Gatwick on 21 March 2026, travelling via Ascend Airline on a six-hour direct flight to Banjul International Airport, and returned on 28 March 2026. GamMed is a registered UK charity (No. 1191320), established in 2017 to provide sustainable surgical care and education in The Gambia, a country of 2.6 million people with an HDI ranking of 174 and limited access to complex surgical services. The mission was led by Mr Kyle James (Consultant Orthopaedic Surgeon) and Mr Tomas Tickunas (Consultant Plastic Surgeon), supported by a multidisciplinary team of 17 clinicians over six intensive days at Edward Francis Small Teaching Hospital (EFSTH), Banjul. The team assessed 135 patients and performed 43 surgical procedures across orthopaedics, plastic surgery, burns reconstruction, and — for the first time on this mission — microsurgical free flap reconstruction.

The Team
Mission Leads: Mr Kyle James – Consultant Orthopaedic Surgeon | Mr Tomas Tickunas – Consultant Plastic Surgeon
BFIRST Contributor: Mr Ahmed Emam – Consultant Plastic & Reconstructive Surgeon, Swansea Bay University Health Board (Orthoplastic Surgery & Microsurgery)
Host Institution: Edward Francis Small Teaching Hospital (EFSTH), Banjul, The Gambia — in collaboration with local surgical and nursing teams.
Clinical Overview
The mission encompassed a broad spectrum of pathology rarely seen in volume in the UK, including bone infections, complicated trauma with bone loss, congenital deformities, and burn contractures affecting both children and adults. The breadth and complexity of cases underscored the significant unmet surgical need in The Gambia and the critical role that visiting specialist teams play in supplementing local capacity.
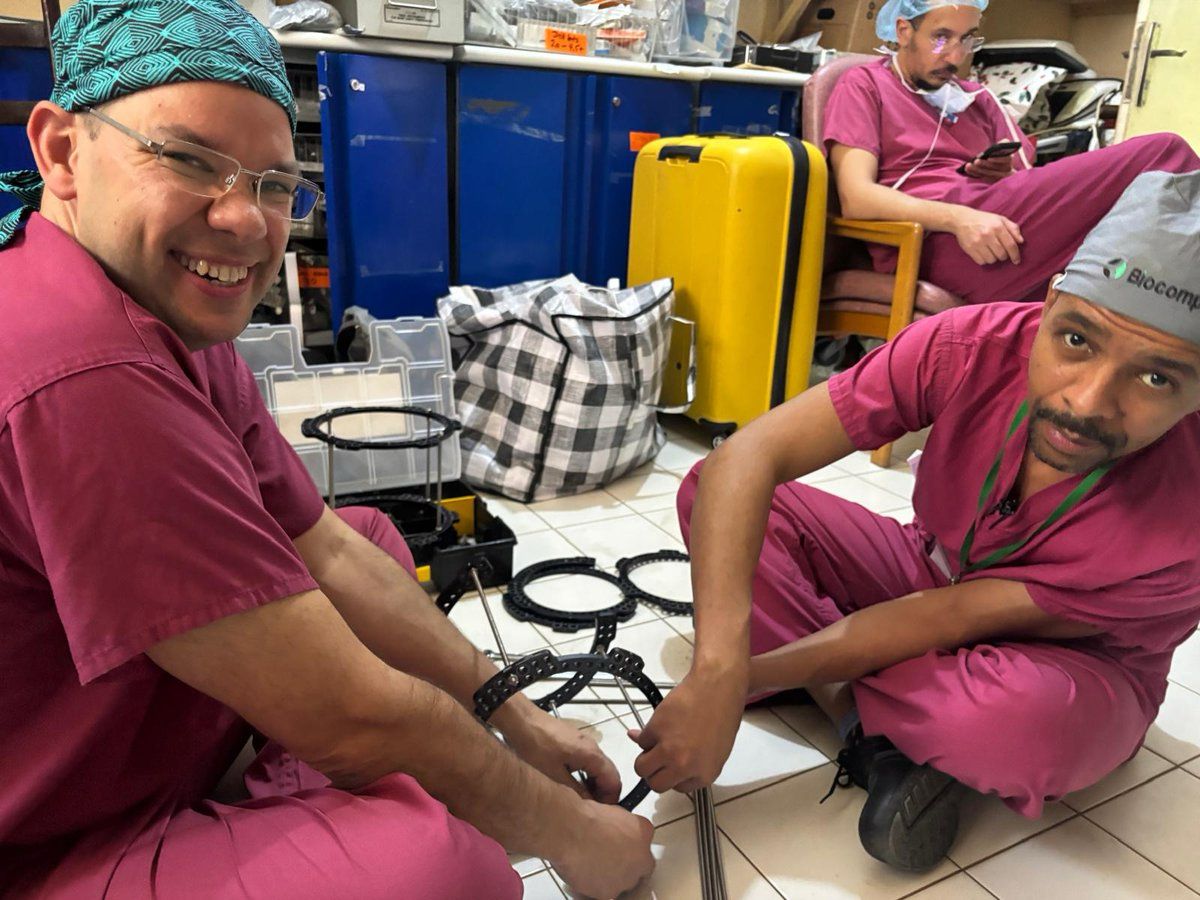
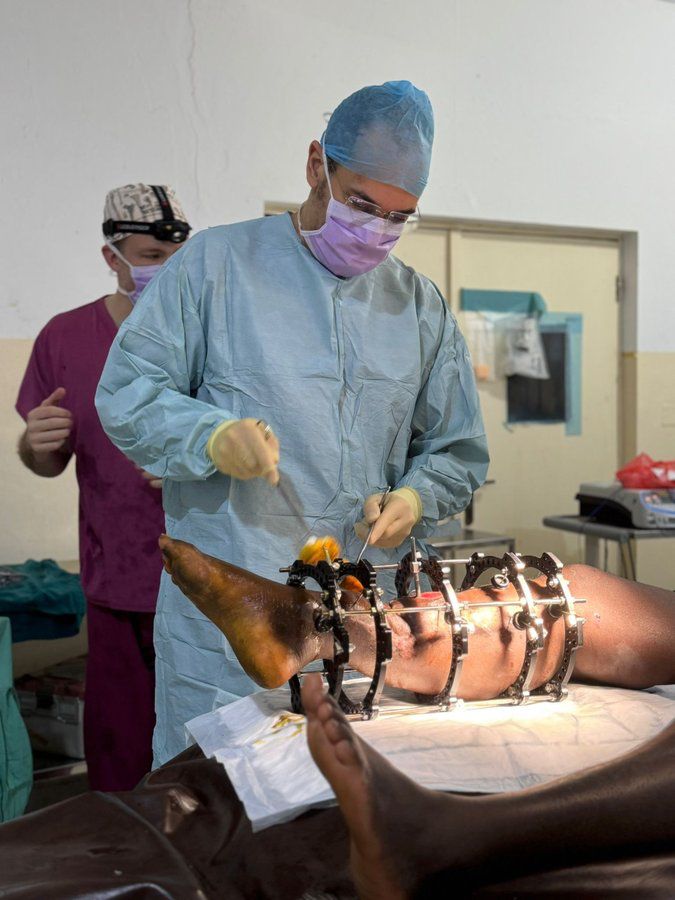
Microsurgical Free Flap Reconstruction — A Historic First
The most clinically significant and technically demanding case of the mission involved a 17-year-old female presenting with a severely comminuted open tibial fracture of the left leg. The wound had remained open for seven weeks prior to the mission. Preoperative imaging – doppler - confirmed a single-vessel limb — a profoundly hostile reconstructive environment — with extensive soft tissue loss overlying the fracture site and 15 cm segmental bone loss. Free flap reconstruction was the only viable option to salvage the limb and avoid amputation.
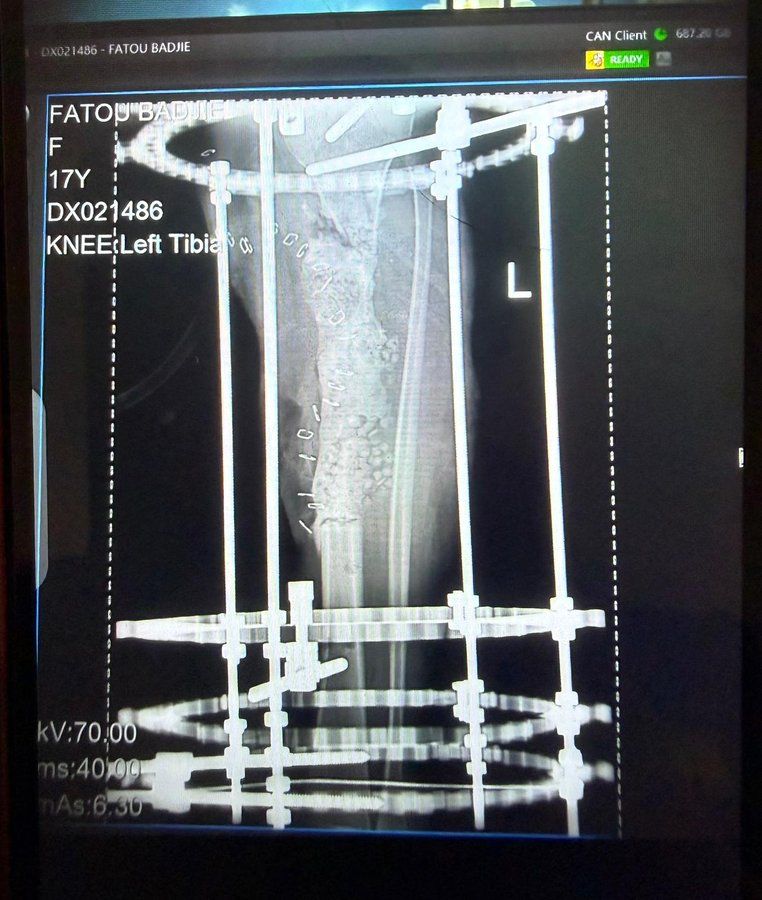
The Operation
Operating under the Zeiss surgical microscope available at EFSTH that was found not used in the hospital and was checked preoperatively and made sure it is functioning — a single-operator instrument without assistant binocular access — a free flap reconstruction was performed. Personal microsurgical instruments brought from the UK were used, including microsutures carried by the operating surgeon. A vein graft was incorporated to bridge the vascular defect created by the single-vessel anatomy. An old bipolar coagulation machine was donated to the hospital to support future cases.
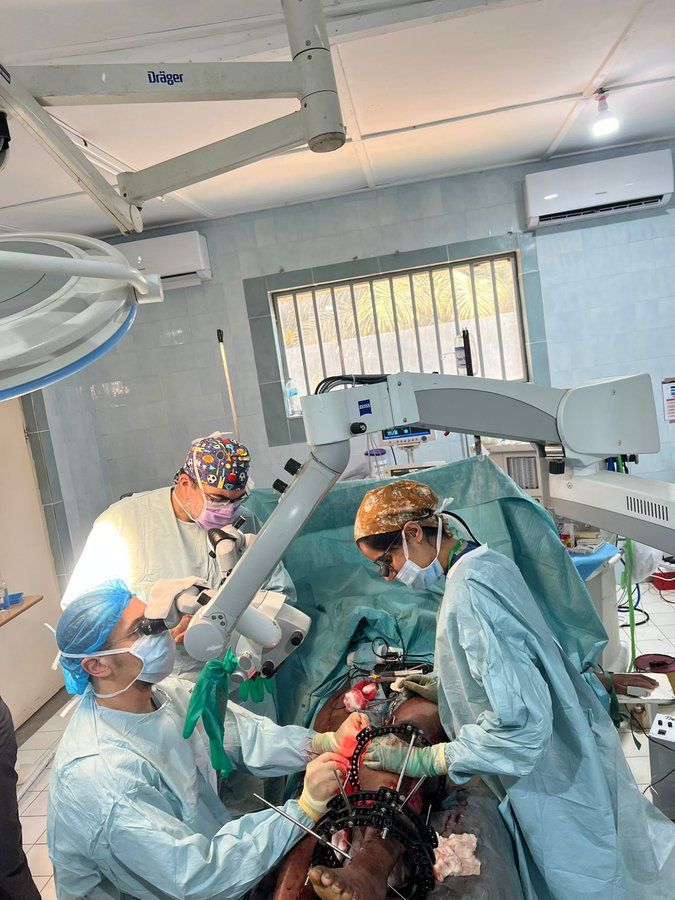
Postoperative Course and Flap Compromise
The immediate postoperative period highlighted the critical infrastructure gaps that currently preclude routine microsurgery in The Gambia. Structured flap monitoring protocols do not exist at EFSTH, and dedicated postoperative nursing observation for vascular compromise is unavailable. On postoperative days one and two, the patient was transported — against explicit medical instruction — to a separate hospital facility for plain radiographs, exposing the limb to uncontrolled positioning and pressure. On day three, the patient was found lying directly on the vein graft on the open ward, causing positional compression of the anastomosis. This led to compromise of the flap.
This outcome, whilst deeply disappointing, does not reflect a failure of operative technique. Rather, it illustrates with clarity that microsurgery cannot yet be delivered safely and routinely in The Gambia without targeted investment in postoperative infrastructure and staff education.
Current Microsurgery Capability Assessment
This mission provided the first structured opportunity to assess the baseline microsurgical infrastructure at EFSTH and to identify the specific gaps that must be addressed before free flap reconstruction can be offered reliably.
What Is Already Present
- Operating Microscope: A Zeiss surgical microscope is available and functional — however it is single operator with no assistant eyepiece, limiting teaching and task-sharing.
- Operating Microscope: A Zeiss surgical microscope is available and functional — however it is single operator with no assistant eyepiece, limiting teaching and task-sharing.
- Operating Theatre: EFSTH has a functioning theatre with anaesthetic support capable of delivering general anaesthesia but not for extended cases due to lack of Co2 monitoring but the skills of the block anaesthetist allowed prolonged procedures to be carried out under regional anaesthetsia.
- Surgical Enthusiasm: The local surgical team demonstrated genuine willingness to engage with microsurgical cases and to develop this capability.
- Ilizarov Fixation Expertise: The orthopaedic team has established Ilizarov frame skills — an essential component of the orthoplastic approach to complex tibial reconstruction.
Critical Gaps Identified
- Dual-Operator Microscope: The current single-operator microscope is insufficient. A dual-head microscope with assistant binoculars is essential for safe task-sharing during anastomosis.
- Microsurgical Instrument Set: Only personal instruments were available. A dedicated quality microsurgical set — including Acland clamps, jeweller's forceps, microneedle holders — must be kept with the visiting team.
- Microsutures: No microsutures (9-0 or 10-0 nylon) are available at EFSTH. These must be brought by visiting teams or procured through sponsorship.
- Doppler Probe: A handheld Doppler probe for postoperative flap monitoring is not available. This is non-negotiable for safe free flap surgery.
- Postoperative Monitoring Protocol: There is no structured flap monitoring protocol and nursing staff are not trained to recognise vascular compromise. This is the most critical educational gap and was directly implicated in the flap compromise on this mission.
- Dedicated Postoperative Space: Free flap patients cannot be safely cared for on an open ward. A single dedicated monitored bed with trained nursing oversight for the first 72 hours is essential.
- Patient Education and Compliance: Patients and families must be counselled preoperatively about immobility requirements. On-site radiography would prevent dangerous inter-hospital transfers in the early postoperative period.
Investment Required to Establish Safe Microsurgery
Free flap microsurgery in The Gambia is technically feasible — the clinical need is real and urgent. What is required is a targeted, phased investment in equipment, education, and systems. The table below outlines the minimum investment needed to make microsurgery safe and deliverable on future GamMed missions.
| Item |
Specification / Notes |
Priority |
Est. Cost (GBP) |
| Dual-operator operating microscope |
Leica or Zeiss with assistant binoculars; travels with team |
Low |
£15,000 - £35,000 (refurbished) |
| Microsurgical instrument set |
Acland clamps, jeweller's forceps, needle holders, dilators — kept with team |
Essential |
£2,000 - £4,000 |
| Microsutures (9-0 / 10-0 nylon) |
Per-mission supply; sponsor to fund annual supply |
Essential |
£500–£800 per mission |
| Handheld Doppler probe |
Portable; kept at EFSTH for postoperative monitoring |
Essential |
£200–£400 |
| Flap monitoring training programme |
Nursing and junior doctor education; bedside monitoring charts; simulation models |
Essential |
£500–£1,000 |
| Dedicated postoperative observation space |
Single monitored bed with pulse oximeter and call system |
High |
£1,000 £2,000 |
Learning Points and Recommendations
When Is Free Flap Surgery Justified?
Microsurgical free flap reconstruction in a resource-limited setting is not appropriate for routine use, but it remains the only reconstructive option in a defined subset of patients — those with single-vessel limbs, large soft tissue defects over bone, post-traumatic or post-infective wounds with exposed hardware, and cases where amputation would otherwise be inevitable. For these patients, free flap reconstruction is the sole pathway to limb salvage. Withholding it on the grounds of resource limitation condemns them to avoidable disability.
Recommendations for Future Missions
- Invest in a dual-operator operating microscope that travels with the GamMed team. This is the single most important enabling step.
- Develop a structured flap monitoring education programme, delivered in person on each mission and reinforced with printed bedside protocols.
- Appoint a local clinical champion — ideally a senior nurse or junior doctor — responsible for flap monitoring continuity between missions.
- Ensure all microsurgical instruments and sutures travel with the visiting team and are not left at the hospital between missions.
- Provide preoperative patient and family education regarding postoperative restrictions, with the support of local staff and translators.
- Approach BFIRST and potential sponsors with a costed proposal for microsurgery capability development. The clinical need is unambiguous, the investment is modest, and the impact is potentially limb- and life-saving.
- Consider pairing future microsurgical cases with a dedicated in-country supervisor who remains with the patient for the first 72 postoperative hours, until nursing monitoring capability is established.
Achievements of This Mission
- First microsurgical free flap attempted in The Gambia within the GamMed programme
- 135 patients assessed; 43 surgeries performed across multiple specialties
- 35+ local medical professionals engaged in education and training
- Donation of bipolar diathermy equipment to EFSTH
- Detailed infrastructure assessment for future microsurgery development
- Engagement with a potential sponsor interested in funding microsurgical capability
- Strengthening of the orthoplastic model within the GamMed mission framework
Personal Reflection
Joining the GamMed mission at the invitation of the BFIRST Chairman, Mr Tony Barabas, was a privilege that brought into sharp focus both the extraordinary resilience of surgical teams working in resource-constrained environments, and the profound responsibility that visiting specialists carry. To be able to offer a 17-year-old girl a meaningful chance at limb salvage — a chance that would simply not exist without a visiting microsurgeon — is precisely the kind of clinical impact that global surgery is designed to deliver. The outcome of this case was not the one we had hoped for. But the learning is unambiguous: the technical components of microsurgery can be transported to The Gambia. The human and structural infrastructure to support them cannot yet be assumed. That is the gap BFIRST and its sponsors have the opportunity to close. The GamMed team is exceptional. The commitment of Kyle James, Tomas Tickunas, and their colleagues to sustainable surgical development in The Gambia — year on year — is both inspiring and effective. I look forward to returning as part of this collaboration and to building on the foundations laid in March 2026.
The Path Forward: Building a Sustainable Microsurgery Programme
Chairman’s Remarks
Mr Tony Barabas, Chairman of BFIRST, has reflected on this mission with genuine enthusiasm and a clear strategic perspective. He has noted with regret that Dr Amadou Jallow — the Gambian surgeon BFIRST is actively supporting to become The Gambia’s first plastic surgeon — was not present for this mission. Dr Jallow attended both previous GamMed trips, which were focused on hands and burns surgery. For this mission, with its landmark microsurgical component, his attendance would have been of exceptional educational value.
Dr Amadou Jallow — The Gambia’s First Plastic Surgeon in Training
Dr Amadou Jallow is a Gambian doctor currently undertaking plastic surgery training in Dar es Salaam, Tanzania. BFIRST has funded a two-month fellowship for him at the Ganga Hospital — one of the world’s foremost centres for microsurgical reconstruction — specifically to develop microsurgical skills. He is expected to return to The Gambia at the end of 2026 or in early 2027. Both the Gambian Deputy Minister of Health and the Head of Edward Francis Small Teaching Hospital have verbally committed to establishing a Plastic Surgery department or division within EFSTH upon Dr Jallow’s return. This commitment, at the highest levels of government and institutional leadership, transforms the programme from aspiration into a credible and time-bound objective. The infrastructure investment detailed in this report — the equipment, the monitoring protocols, the education programme — is precisely what is needed to ensure that Dr Jallow returns to an environment in which he can practice safely and effectively from day one. The alignment of these threads is significant: a trained Gambian microsurgeon returning home, a government-level commitment to a plastic surgery division, and a documented, costed infrastructure gap that sponsors can directly address. A targeted investment now does not merely support a single mission — it seeds a permanent surgical capability in a country that currently has none.
Dr Daniel Aboye — A Potential Second Pillar
Dr Daniel Aboye, from Ethiopia, may also join Dr Jallow in The Gambia at a similar time, should the Gambian Department of Health fulfil its expressed intention to invest in a dedicated burns unit. The potential co establishment of a plastic surgery division and a burns unit — delivered by two internationally trained surgeons with BFIRST-supported fellowships — represents a programme of impact that is rare in global surgery: not an episodic visiting mission, but the creation of an enduring in-country capacity. This report, and the costed investment proposals it contains, is submitted with the dual purpose of informing BFIRST’s strategic planning and providing the evidence base for engagement with prospective sponsors. The clinical need is unambiguous, the institutional will is present, and the human resource — a Gambian-trained microsurgeon — is within reach. What remains is the infrastructure to receive him.
Conclusion
Microsurgical free flap reconstruction has been demonstrated to be technically feasible within the GamMed mission framework. It is needed in a clearly defined and clinically significant subset of patients for whom no other reconstructive option exists. Establishing it safely requires targeted but achievable investment — principally a dual-operator operating microscope, a quality instrument set, and a structured flap monitoring education programme. The total capital investment is modest relative to the impact it would enable. BFIRST is well positioned to facilitate this development, both through direct support and through engagement with sponsors who share an interest in advancing microsurgery in low- and middle-income settings. The convergence of factors is unusually favourable: a Gambian surgeon — Dr Amadou Jallow — trained in microsurgery and due to return home by the end of 2026; a government-level commitment to establish a Plastic Surgery division at EFSTH; and a clearly costed, achievable infrastructure gap. This report is submitted as the evidence base for that conversation — and as a foundation for engagement with sponsors whose investment can help realise a permanent surgical legacy in The Gambia.
Mr Ahmed Emam
Consultant Plastic & Reconstructive Surgeon
Swansea Bay University Health Board
Co-Chair, BFIRST Education, Research & Fellowship Subcommittee
April 2026