BFIRST April Newsletter 2026
01 May 2026
(Last updated: 1 May 2026 11:15)
BFIRST is a UK registered charity which trains surgeons and their teams working in low to middle income countries to enable them to undertake reconstructive Plastic Surgery independently in an equitable and sustainable manner. Treating functional disability, injury and pathology via surgical treatment helps enable restoration of independence to both adults and children thereby improving quality of life.
BFIRST also provides educational resources for Plastic and Reconstructive Surgeons through our Webinar series.
In the April 2026 BFIRST newsletter we bring you up to date with our latest activities undertaken by BFIRST and hope that they inspire you to get involved!

BFIRST Essay Prize
BFIRST Essay Prize (£250.00) 2026
We are delighted to announce the 2026 BFIRST Essay Prize!
The title for this year’s contest is “How can harnessing AI transform surgical care in resource-poor countries – for better or worse?”
We are looking forward to receiving your essay until 23.59 GMT, on 1 May 2026.
Please follow this link for more details!
This month we welcome Alan Neffy as the new treasurer for BFIRST! He is featured in this month’s meet the team.
Meet the Team
 Tell us about yourself!
Tell us about yourself!
My name is Terouz, meaning “sunshine.” I am the National Surgical Innovation Fellow at the Royal College of Surgeons of England, having a background of a plastics-themed core surgical training in London. I combine clinical work with medical illustration and innovation, focusing on turning ideas into real-world impact. My aim is to support a more equitable surgical system, where high-quality care is accessible to all.
Tell us about your time with BFIRST
I was introduced to BFIRST as a medical student after winning their essay prize and presenting at Overseas Day—an experience that shaped my outlook. I was struck by its collaborative, equity-focused ethos and commitment to long-term partnerships. Since then, I’ve contributed to BFIRST work in Tanzania, published in global surgery, and developed a country prioritisation tool. BFIRST has remained a key influence, shaping my view of global surgery as integral to good surgical practice.
Why did you want to work with BFIRST?
My motivation for medicine, particularly plastic surgery, is shaped by my background as a Kurdish refugee and early exposure to unequal healthcare access. I was drawn to BFIRST for its focus on sustainable, partnership-based global surgery and capacity building. Through it, I aim to develop both technical skill and the ability to contribute meaningfully in low-resource settings. This blend of clinical excellence and systems thinking continues to drive my involvement.
What are your aspirations for BFIRST?
BFIRST already delivers high-quality training and long-term partnerships; my aim is to see its impact amplified. There’s an opportunity to better capture and share its learning, strengthening its role as a thought leader in global surgery. I’d also like to see deeper collaboration with academia, industry, and NGOs to scale impact sustainably. Ultimately, BFIRST can shape both its trainees and the broader vision of equitable surgical care.
What do you like to do outside of work and BFIRST?
Outside of work, I’m an artist and medical illustrator. Drawing anatomy has deepened my understanding of structure and evolved into creating educational resources, including an upper limb series used in UN Global Surgery Training Hub modules.
What began as a personal practice now contributes to surgical education at scale. I see art and surgery as closely linked through precision and observation, and I also enjoy the outdoors, especially mountains and cycling.
Webinars
BFIRST 2026 Webinar Series
Please follow our socials for updates about future webinars.
If you have missed any of the webinars from last year, you can watch them on our website including some fantastic webinars for revision of key topics within Plastic Surgery!
Our previous webinars are now also available via our YouTube channel!
Projects
Peru: A BFIRST badged visit

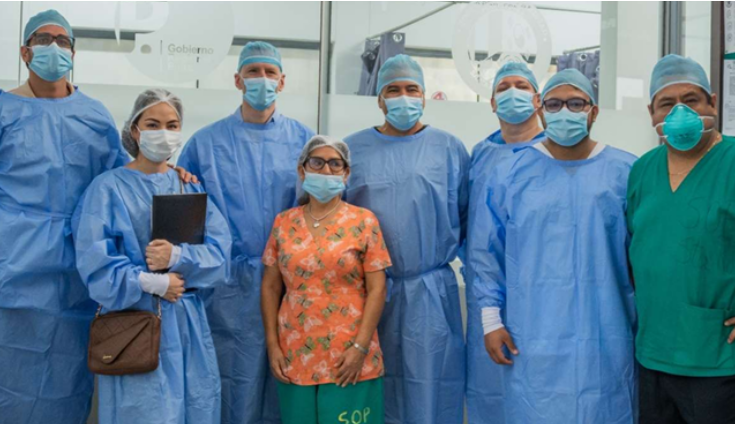
Outside Hospital Santa Rosa. Left to Right: Mr Alderson, Dr Santivanez, Mr Barabas, Ms De La Cruz Monroy
Scoping Trip Report Summary – Project UKallpa (March 2026)
 Project UKallpa is a UK–Peru surgical outreach and education initiative led by UK-based plastic surgery trainee Ms Martha De La Cruz Monroy, in collaboration with EcoSwell and BFIRST. The project aims to strengthen reconstructive surgical care in Peru through hands-on clinical work, training, and long-term capacity building at two key hospitals: Hospital Santa Rosa II-2 in Piura and Hospital Arzobispo Loayza in Lima.
Project UKallpa is a UK–Peru surgical outreach and education initiative led by UK-based plastic surgery trainee Ms Martha De La Cruz Monroy, in collaboration with EcoSwell and BFIRST. The project aims to strengthen reconstructive surgical care in Peru through hands-on clinical work, training, and long-term capacity building at two key hospitals: Hospital Santa Rosa II-2 in Piura and Hospital Arzobispo Loayza in Lima.
A scoping visit (23–27 March 2026) was undertaken by a UK multidisciplinary team, including BFIRST chair Mr Tony Barabas, to assess clinical need, infrastructure, and feasibility for a planned outreach mission in November 2026. The visit confirmed a significant unmet surgical need in both regions, with particularly high deprivation and service gaps identified in Piura.
Photo: Left to Right: Ms De La Cruz Monroy, Mr Barabas, Ms Paucar (head of theatre nursing), Dr Santivanez, Dr Leon, Dr Zavala (general surgery resident), Dr (head of operating theatres).
Key Findings
 Hospital Santa Rosa in Piura emerged as the primary focus for intervention. It is the only public tertiary hospital serving approximately 1.4 million people, operating at high capacity with around 400 surgeries per month and frequent ICU saturation. Despite a committed local team, major limitations were identified in microsurgical capability, specialist hand surgery, and reconstructive services. Critical gaps include lack of microsurgery, limited instrument availability, and insufficient consumables such as fine sutures and specialised hand sets. Patients with complex trauma or limb-threatening injuries often face long-distance referral to Lima, with significant risk of disability or amputation if transfer is not possible.
Hospital Santa Rosa in Piura emerged as the primary focus for intervention. It is the only public tertiary hospital serving approximately 1.4 million people, operating at high capacity with around 400 surgeries per month and frequent ICU saturation. Despite a committed local team, major limitations were identified in microsurgical capability, specialist hand surgery, and reconstructive services. Critical gaps include lack of microsurgery, limited instrument availability, and insufficient consumables such as fine sutures and specialised hand sets. Patients with complex trauma or limb-threatening injuries often face long-distance referral to Lima, with significant risk of disability or amputation if transfer is not possible.
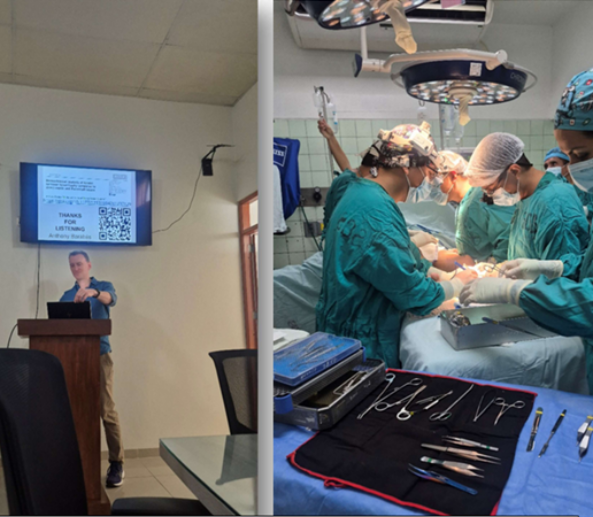
Photo: Left: hand surgery talk by Mr Barabas, Right: complex lower limb reconstructive procedure (free ALT flap + bone graft to left foot)
The hospital has strong willingness to develop services, including potential introduction of microsurgical techniques, supported by UK training input. Theatre infrastructure is available, including four operating theatres, with scope to dedicate additional capacity for visiting teams. Training needs span junior residents and established surgeons, particularly in tendon repair, trauma reconstruction, wound care, and emerging microsurgical skills.
 Photo: At a meeting with the Hospital's Medical Director, Dr Oscar Requena
Photo: At a meeting with the Hospital's Medical Director, Dr Oscar Requena
In contrast, Hospital Arzobispo Loayza in Lima is a major national referral centre with established expertise in microsurgery, burns, and complex reconstruction. It has a high surgical volume (10,000–12,000 procedures annually) and a well-developed plastic surgery department, including a tissue engineering laboratory.
This site offers strong opportunities for academic exchange, resident teaching, and advanced case discussion rather than foundational service delivery.
November 2026 Outreach Plan
 The proposed project involves an 8-person UK surgical team delivering combined clinical service and education across both sites.
The proposed project involves an 8-person UK surgical team delivering combined clinical service and education across both sites.
The programme will prioritise Santa Rosa for operative lists and hands-on training, supported by structured outpatient assessment, five operating theatre days, and dedicated teaching sessions. Lima will focus on knowledge exchange, joint operating, and resident education.
Left: visiting the tissue engineering laboratory. Right: Plastic Surgery ward round
Next Steps
Key milestones include case selection and team confirmation by mid-2026, finalisation of equipment procurement by July, and full multidisciplinary planning by September 2026.
EcoSwell will continue to support logistics, regulatory approvals, and local coordination.
 Photo: Outpatient department area at a secondary site of Santa Rosa Hospital
Photo: Outpatient department area at a secondary site of Santa Rosa Hospital
Conclusion
The scoping visit confirmed both the urgency of need and the strong potential for sustainable impact. Project UKallpa aims not only to deliver reconstructive surgery, but to establish lasting educational and clinical capacity, particularly in Piura, ensuring longer-term self-sufficiency in complex surgical care.
The Gambia: A GamMed project, with BFIRST member Mr Emam

The GamMed March 2026 team outside Edward Francis Small Teaching Hospital, Banjul
BFIRST Report Summary – GamMed Mission, The Gambia (March 2026)
 In March 2026, a UK multidisciplinary surgical team, including BFIRST Education, Research & Fellowship Subcommittee co-chair Mr Ahmed Emam, participated in the GamMed humanitarian mission at Edward Francis Small Teaching Hospital (EFSTH) in Banjul, The Gambia. The programme, delivered under the GamMed UK charity (est. 2017), brought together 17 clinicians to provide reconstructive surgical care and training in a country of 2.6 million people with severely limited access to specialist services.
In March 2026, a UK multidisciplinary surgical team, including BFIRST Education, Research & Fellowship Subcommittee co-chair Mr Ahmed Emam, participated in the GamMed humanitarian mission at Edward Francis Small Teaching Hospital (EFSTH) in Banjul, The Gambia. The programme, delivered under the GamMed UK charity (est. 2017), brought together 17 clinicians to provide reconstructive surgical care and training in a country of 2.6 million people with severely limited access to specialist services.
Over a six-day clinical programme, the team assessed 135 patients and performed 43 operations across orthopaedics, plastic surgery, burns, and reconstructive surgery. The case mix reflected significant unmet need, including chronic osteomyelitis, complex trauma with bone loss, congenital deformities, and burn contractures affecting both adults and children. The mission highlighted the essential role of visiting teams in supplementing local surgical capacity in low-resource settings.
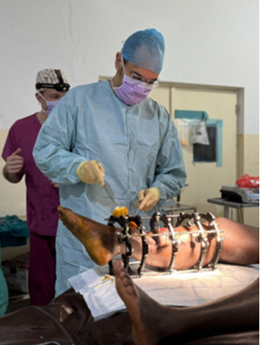
Photo: Prepping Ilizarov frame components prior to surgery
A major milestone was the first attempted microsurgical free flap reconstruction performed within the GamMed programme. The case involved a 17-year-old patient with a severely comminuted open tibial fracture, extensive soft tissue loss, and a single-vessel limb. A limb-salvage free flap was performed using a Zeiss operating microscope available at EFSTH and microsurgical instruments brought from the UK. Despite technically successful surgery and vein graft reconstruction, the flap later failed due to postoperative complications linked to inadequate monitoring, ward infrastructure, and patient handling.
 This outcome provided a clear and important insight: while microsurgical capability can be delivered intraoperatively, safe outcomes depend heavily on postoperative systems that are currently lacking. Key gaps identified include absence of structured flap monitoring protocols, lack of trained nursing surveillance, no dedicated postoperative beds, and insufficient patient education and compliance with immobility requirements.
This outcome provided a clear and important insight: while microsurgical capability can be delivered intraoperatively, safe outcomes depend heavily on postoperative systems that are currently lacking. Key gaps identified include absence of structured flap monitoring protocols, lack of trained nursing surveillance, no dedicated postoperative beds, and insufficient patient education and compliance with immobility requirements.
Photo: Ilizarov Frame application for complex tibial reconstruction
The mission therefore undertook a detailed assessment of microsurgical readiness at EFSTH. Strengths included an available operating microscope, functional theatre capacity, and strong engagement from local surgeons. However, critical deficits were identified, including the need for a dual-operator microscope, microsurgical instrument sets, consistent access to 9–10/0 sutures, a handheld Doppler for flap monitoring, and dedicated postoperative care facilities.
Importantly, the report concludes that microsurgery is clinically justified in The Gambia for carefully selected limb-threatening cases, but cannot yet be delivered safely at scale without targeted investment. Key recommendations include establishing structured flap monitoring training for nurses and junior doctors, introducing standardized postoperative protocols, ensuring all microsurgical consumables are mission-supplied, and developing a local clinical champion to maintain continuity between visits. The creation of a monitored postoperative bed space was identified as essential.
 Beyond the clinical findings, the mission delivered 43 surgeries, extensive education to local staff, and the first structured evaluation of microsurgical potential in-country. It also strengthened collaboration between GamMed, BFIRST, and EFSTH leadership, with growing institutional support for long-term development.
Beyond the clinical findings, the mission delivered 43 surgeries, extensive education to local staff, and the first structured evaluation of microsurgical potential in-country. It also strengthened collaboration between GamMed, BFIRST, and EFSTH leadership, with growing institutional support for long-term development.
A key strategic development is the anticipated return of Dr Amadou Jallow, the first Gambian surgeon undergoing plastic surgery training with BFIRST support, expected in 2026–27. National and hospital leadership have expressed commitment to establishing a plastic surgery division at EFSTH upon his return. The report positions current investment in microsurgical infrastructure as critical to enabling this future service.
Overall, the March 2026 mission demonstrates both the feasibility and the limitations of advanced reconstructive surgery in low-resource settings. It reinforces a central conclusion: lasting impact depends not only on surgical expertise, but on building the systems required to support it safely.
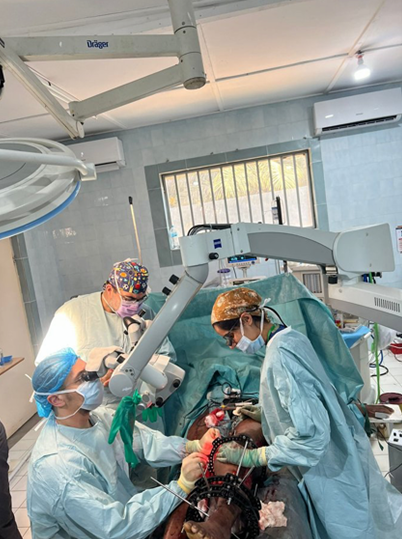
Photo: Intraoperative view: microsurgical free flap reconstruction under the Zeiss operating microscope at ESFTH. Mr Emam (left, at microscope) and Mr Tickunas assisting.
A key focus of this mission was laying the educational and structural foundations for sustainable surgical training in The Gambia. Whilst the absence of local plastic surgery specialists at this stage reflects the very gap that BFIRST exists to address, the mission provided a unique opportunity to assess the training environment, engage with local clinical staff, and document the infrastructure requirements that will be essential when in-country plastic surgery capacity is established. Valuable nursing education and patient care training was delivered throughout the week by the wider mission team. BFIRST's longer-term contribution to skills transfer in The Gambia is already in motion through its active support of a Gambian surgeon currently undertaking specialist plastic surgery and microsurgery training abroad, with a planned return to establish the country's first plastic surgery service. The groundwork laid on this mission — clinical, educational, and infrastructural — is designed to ensure that when that moment arrives, the environment is ready to receive it.
Fellowships
BFIRST Fellows
The 2026 BFIRST fellows have been selected, congratulations to:
- Dr Lambert Onahi Iji from Nigeria
- Dr Masroor-ur-Rahman from Bangladesh
Fundraising
We would be grateful for any donations to help support our work.
Tough Mudder

BFIRST are planning to enter a team for Tough Mudder in September, if you are keen to join the BFIRST Tough Mudder team let us know here!
 BFIRST Scrub Hats
BFIRST Scrub Hats
We launched the BFIRST scrub hats at the BAPRAS Congress in December 2025, which were hugely popular, if you would like to purchase a hat please email: hcroberts46@gmail.com.
All proceeds will fund work undertaken by BFIRST!
Easyfundraising
 Raise free funds for BFIRST with your everyday online shopping, visit easyfundraising to get started.
Raise free funds for BFIRST with your everyday online shopping, visit easyfundraising to get started.
When shopping online by signing up to Easyfundraising your purchases will generate free funding for BFIRST!
Other
 Open Hand Therapy Initiative
Open Hand Therapy Initiative
The Open Hand Therapy Initiative aims to improve hand injury care in resource challenged settings in order to reduce disability, improve quality of life and increase chances of work for people with hand injuries and conditions.
They provide accessible, relevant and captivating learning opportunities for generalist occupational therapists and physiotherapists that motivate ongoing development for hand-injury care.
They also invite hand therapists acquainted with the challenges faced in low to middle income countries to participate in strengthening hand injury care in these settings by sharing their expertise.
For more information click here!